What Is a whipple procedure? Understanding your pancreatic surgery options.
Have you or a loved one been told that you need a surgical procedure called a “whipple?”
Pancreatic cancer, a necrotic gallbladder, or bile duct cancer are just a few of the very serious conditions that call for a whipple or modified whipple procedure.
The Whipple procedure is considered the most common surgery for pancreatic cancer, with thousands performed annually in the United States. The Whipple procedure, also known as pancreaticoduodenectomy, is a complex surgical treatment primarily used to remove cancerous tumors within the head of the pancreas. This critical operation also typically involves the removal of part of the small intestine, bile duct, and sometimes additional nearby tissues affected by the cancer. Renowned as a pivotal surgery for treating pancreatic cancer, the Whipple procedure aims to prevent cancer from spreading and to enhance long-term survival chances. Pancreatic cancer, a necrotic gallbladder, or bile duct cancer are just a few of the very serious conditions that call for a whipple or modified whipple procedure.
If you have been told you need a whipple procedure for any reason, you need an experienced, extremely qualified surgeon to perform the surgery. Someone you trust with your life as they are removing organs and “reworking” the flow of the digestive tract.
Such a surgeon can be found at the Southern California Multi-Specialty Center in Los Angeles. For more information contact the specialty center at (818) 900-6480.
If you want to know more about the Whipple procedure and the capabilities of the surgeon doing the work read on. In this article we discuss what pancreatic cancer is, the whipple procedure, conditions treated, what happens before and after the procedure and during recovery time. For more information about the surgeon doing the procedure you can look here for his surgical qualifications.
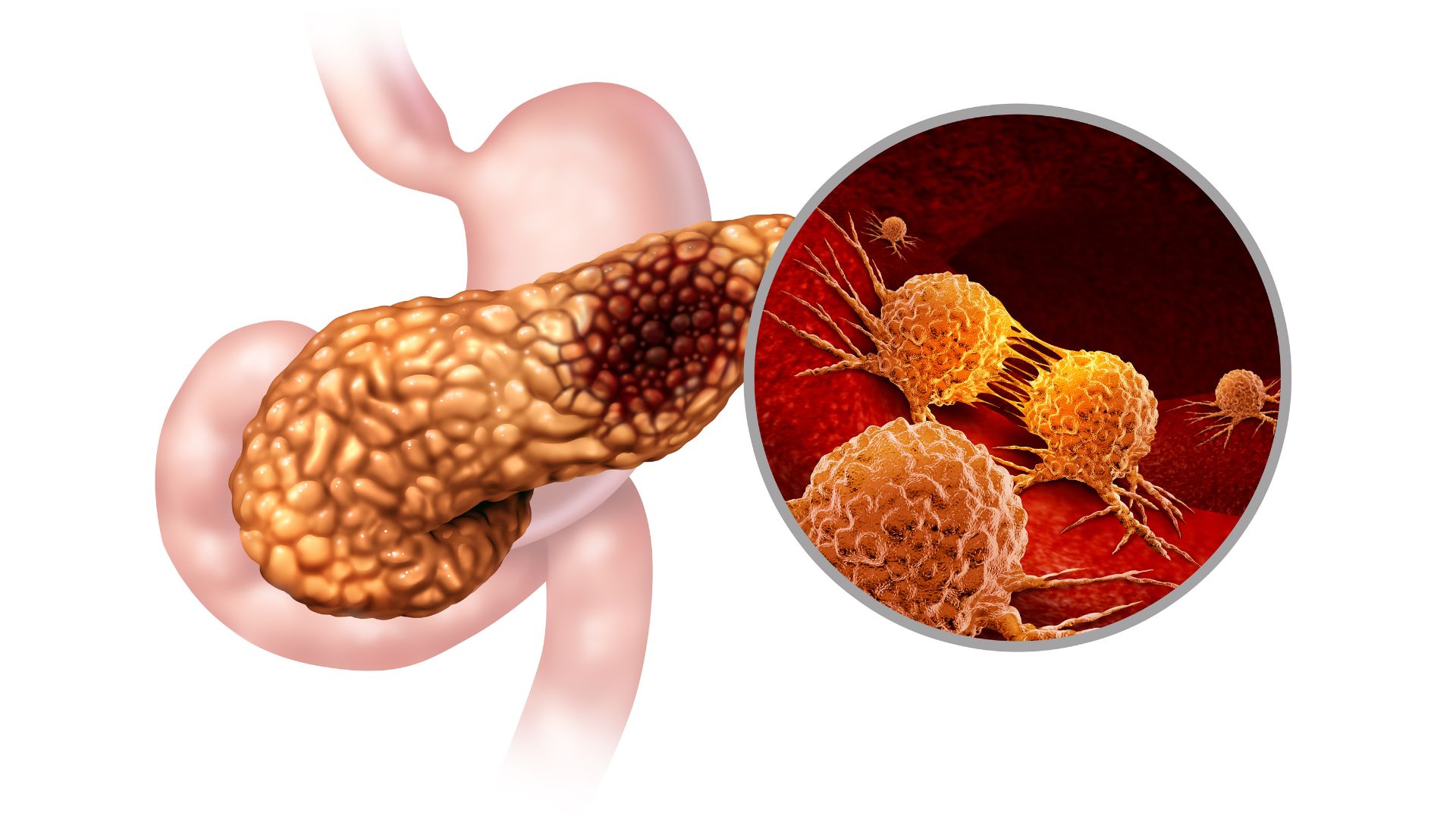
Pancreatic cancer starts in the pancrease and is a serious and often deadly disease. Common symptoms may include abdominal pain, weight loss, jaundice (yellowing of the skin and eyes), and digestive problems such as nausea and diarrhea.
What is Pancreatic Cancer?
Pancreatic cancer is a type of cancer that starts in the pancreas, which is a gland located behind the stomach that produces digestive enzymes and hormones such as insulin and glucagon. Pancreatic cancer occurs when abnormal cells in the pancreas grow and divide uncontrollably, forming a mass or tumor.
Pancreatic cancer is a serious and often deadly disease, with symptoms that may not appear until the cancer is advanced. Common symptoms of pancreatic cancer include abdominal pain, weight loss, jaundice (yellowing of the skin and eyes), and digestive problems such as nausea and diarrhea.
There are several types of pancreatic cancer, including the most common type, pancreatic ductal adenocarcinoma. Other less common types include neuroendocrine tumors and pancreatic acinar cell carcinoma.
Treatment for pancreatic cancer may include surgery, chemotherapy, radiation therapy, or a combination of these approaches. The treatment plan will depend on several factors, including the type and stage of the cancer, the patient’s overall health, and their personal preferences.
Early detection and treatment of pancreatic cancer can improve the chances of successful treatment and long-term survival.
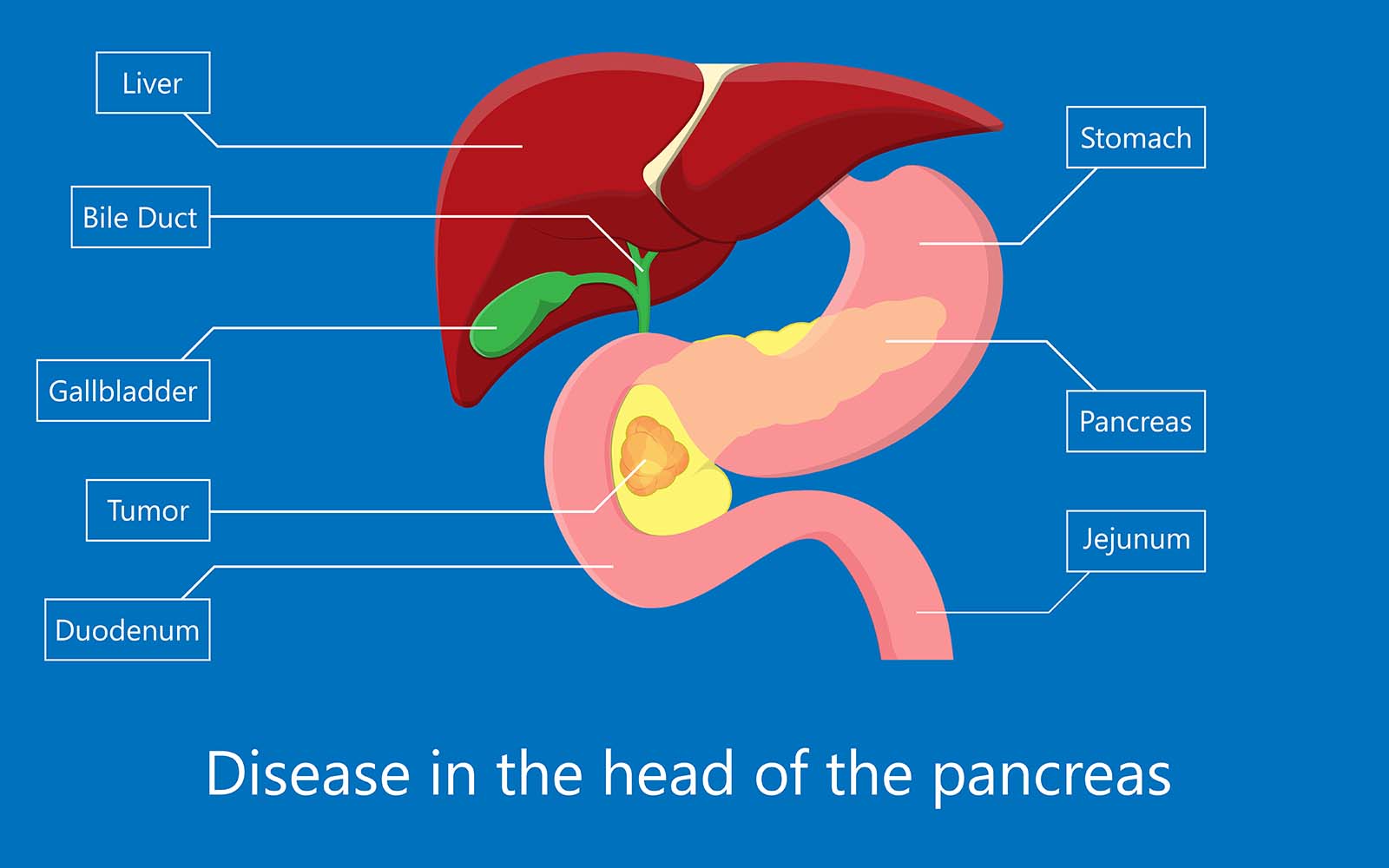
The Whipple procedure is the primary treatment for pancreatic cancer patients
This type of pancreatic cancer surgery is also commonly referred to as a “pancreaticoduodenectomy.” This surgery is also used to treat other tumors or cancer of the pancreas, intestine, and bile duct.
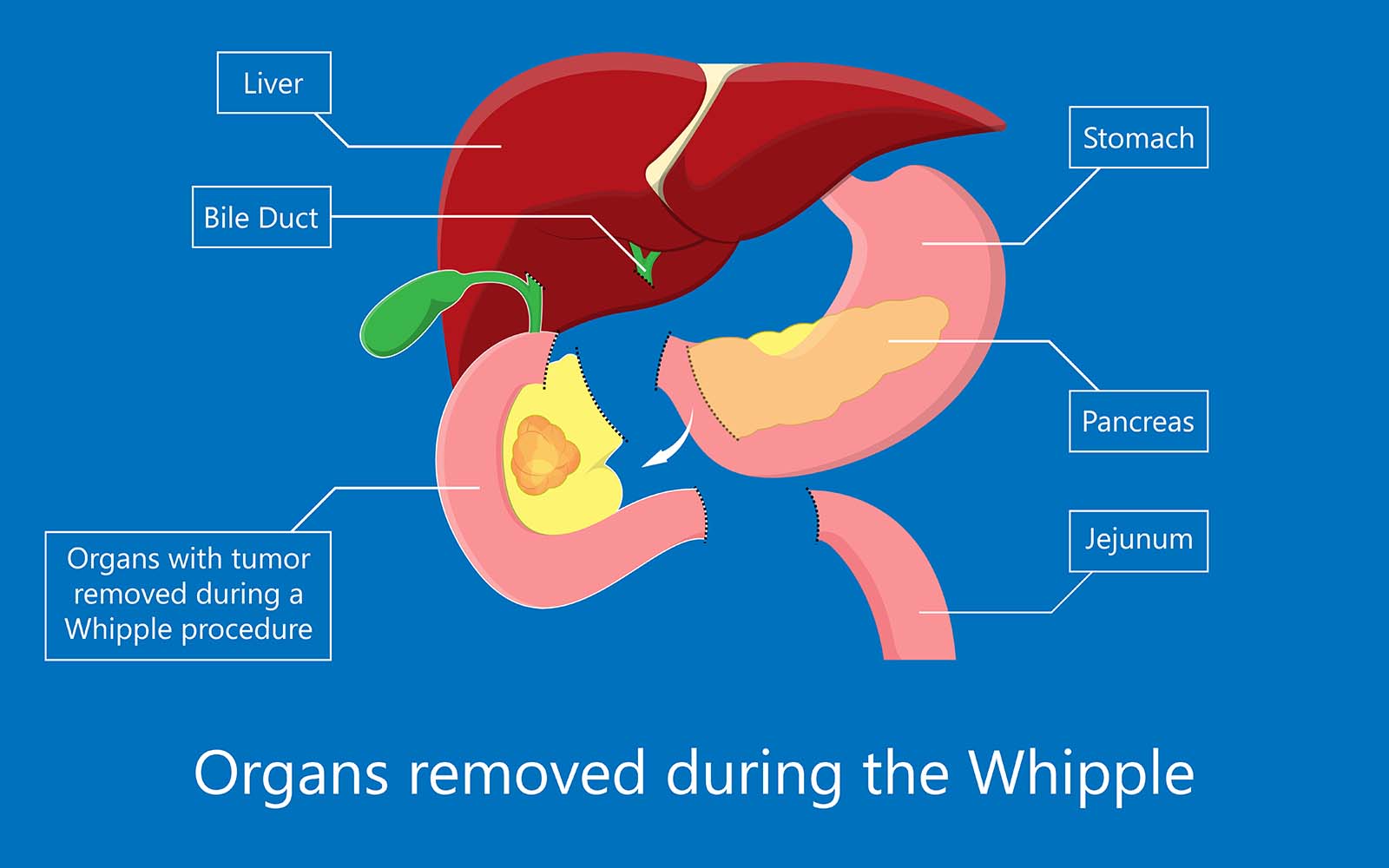
The Whipple procedure is a complex surgery for the surgical team. It removes the head of the pancreas, the first part of the small intestine (duodenum), the gall bladder, the common bile duct, and possibly infected nearby lymph nodes.
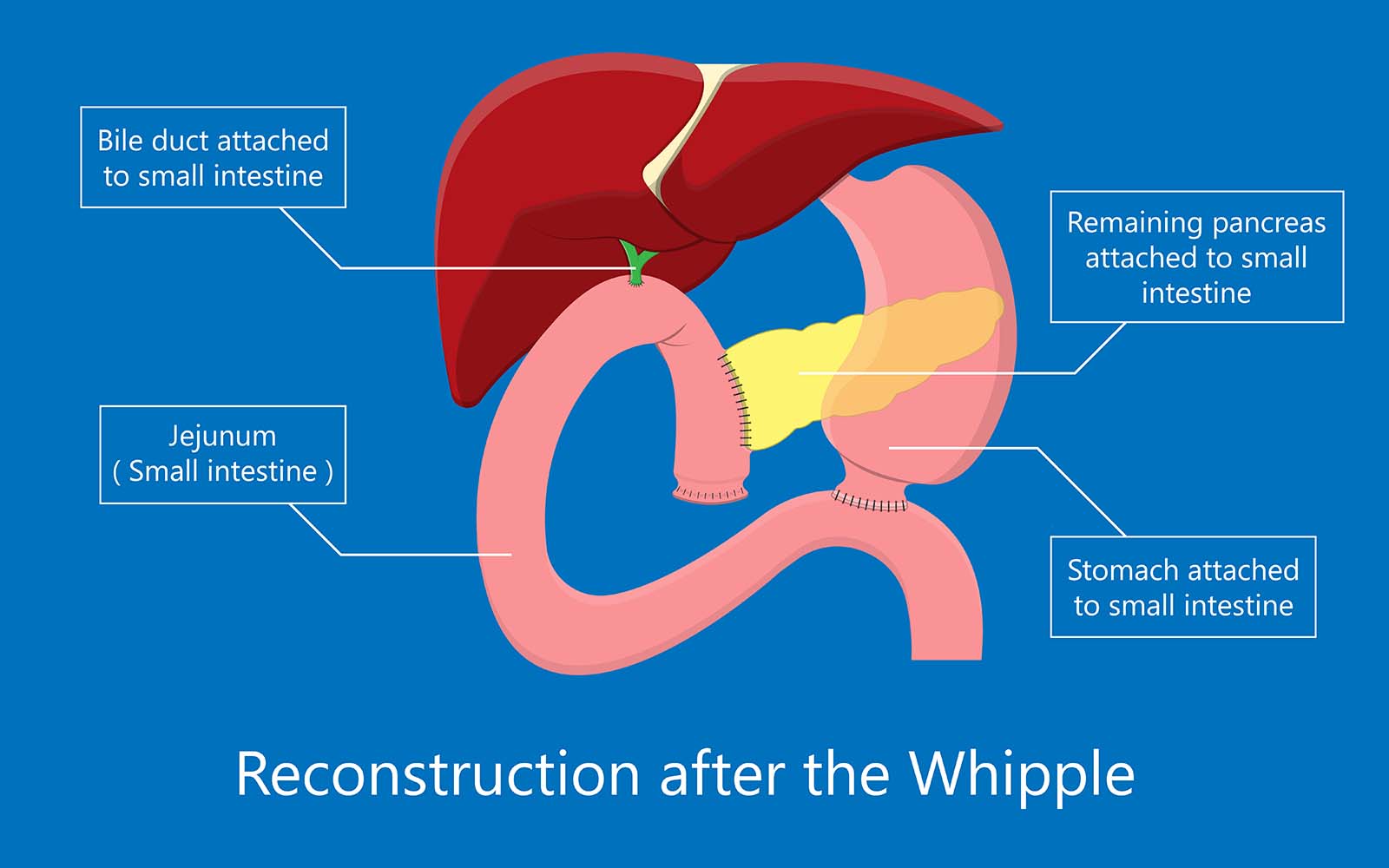
After the organs are partially removed, your surgeon will reconnect the organs to allow you to digest food normally.
This surgery, on average, takes 6 hours to complete. You can expect longer if your case is complex. After surgery, patients spend 1-2 weeks in the hospital for recovery. It is a difficult and demanding operation for the surgeon, it also carries high risks, but in many cases, it is a lifesaving operation for cancer patients.
What to expect when recovering from Whipple surgery
The recovery time after a Whipple surgery can vary depending on the individual patient’s health status and the extent of the procedure. In general, most patients can expect to stay in the hospital for 1-2 weeks following the surgery.
After being discharged from the hospital, the recovery process typically continues for several weeks to months. During this time, the patient may experience fatigue, weakness, and digestive issues. They may also need to follow a special diet and take medication to manage pain and prevent infection.
It is important for patients to follow their healthcare team’s instructions carefully and attend all follow-up appointments to monitor their progress and manage any complications that may arise. With proper care and management, most patients are able to resume normal activities within several months of the surgery. However, it is important to note that every patient’s recovery is unique and the timeline may vary.
Survival rates following a Whipple procedure
Potential Whipple procedure complications
As with any major surgery, a Whipple procedure can carry some risks and potential complications, which may include:
- Bleeding: In rare cases, bleeding may occur during or after the surgery, requiring additional medical intervention.
- Infection: The surgical site or other parts of the body may become infected after the surgery, leading to fever, pain, and other symptoms.
- Pancreatic fistula: This is a leakage of pancreatic juices from the surgical site, which may cause infection or inflammation.
- Delayed gastric emptying: This is a condition in which the stomach is slow to empty, leading to nausea, vomiting, and bloating.
- Digestive problems: The removal of a portion of the digestive tract may cause changes in bowel movements and digestion.
- Diabetes: In rare cases, removal of the pancreas can lead to the development of diabetes.
- Blood clots: Prolonged bed rest and surgery increase the risk of developing blood clots in the legs or lungs.
- Respiratory problems: General anesthesia can cause breathing problems in some patients, particularly those with pre-existing lung disease.
It is important for patients to discuss the potential risks and complications of a Whipple procedure with their healthcare team and weigh them against the potential benefits of the surgery. With proper care and monitoring, most complications can be managed effectively.
Whipple Surgery Q&A
Surgeons can treat pancreatic cancer using the Whipple surgery procedure, also known as a pancreaticoduodenectomy. It may be performed as a traditional open procedure or as a robotic surgery.
Is the Whipple procedure an open or minimally invasive surgery?
The Whipple procedure can be done either as a traditional open procedure or as a robotic surgery which leads to fewer complications. At SCMSC, Dr. Babak Eghbalieh, can offer both options and together decide which option is best for you.
There are many benefits to a robotic approach, if you are considered a good candidate for this. Primarily, the main benefits of robotic surgery compared to open surgery are faster healing and recovery time, less scarring, and decreased pain.
Is the Whipple procedure recommended for all pancreatic cancer patients?
Conditions treated with the Whipple procedure
A Whipple procedure may be a treatment option for people whose pancreas, duodenum (first part of the small intestine) or bile duct is affected by cancer or other disorder. The pancreas is a vital organ that lies in the upper abdomen, behind your stomach.
It works closely with the liver and ducts that carry bile. The pancreas releases (secretes) pancreatic enzymes that help you digest food, especially fats and protein. The pancreas also secretes hormones that help manage your blood sugar.
Your doctor may recommend you have a Whipple procedure to treat:
- Pancreatic cancer
- Pancreatic cysts
- Pancreatic tumors
- Pancreatitis
- Ampullary cancer
- Bile duct cancer
- Neuroendocrine tumors
- Small bowel cancer
- Trauma to the pancreas or small intestine
- Other tumors or disorders involving the pancreas, duodenum or bile ducts
The goal of doing a Whipple procedure for cancer is to remove the tumor and prevent it from growing and spreading to other organs. This is the only treatment that can lead to prolonged survival and cure for most of these tumors.
How will I prepare for a whipple procedure?
Before a Whipple surgical procedure the patient will typically undergo several preoperative preparations, including:
- Medical evaluation: The patient will undergo a comprehensive medical evaluation, which may include blood tests, imaging studies, and other diagnostic tests to assess their overall health status.
- Nutritional assessment: Patients with pancreatic cancer may have difficulty absorbing nutrients, so a nutritional assessment is typically performed to determine if any deficiencies need to be corrected before surgery.
- Bowel preparation: The patient may be given a laxative or enema to empty their bowels before surgery.
- Fasting: The patient will typically be instructed to stop eating and drinking for a certain period before surgery to reduce the risk of aspiration during the procedure.
Consent: The surgeon will explain the risks and benefits of the procedure to the patient and obtain their informed consent before the surgery.
What happens after Whipple surgery?
After a Whipple surgical procedure, the patient will typically remain in the hospital for several days to recover. Here are some of the things that may happen during this recovery period:
- Monitoring: The patient will be closely monitored for any signs of complications, such as bleeding, infection, or organ failure.
- Pain management: The patient will receive pain medication to manage their pain and discomfort.
- IV fluids and nutrition: The patient may receive intravenous (IV) fluids and nutrition if they are not yet able to tolerate oral intake.
- Wound care: The surgical incisions will be monitored and cared for to prevent infection.
- Mobility: The patient will be encouraged to move around as soon as possible after surgery to prevent blood clots and promote healing.
- Follow-up appointments: The patient will need to attend follow-up appointments with their healthcare team to monitor their recovery and manage any complications that may arise.
After leaving the hospital, the patient will need to continue to follow a strict diet and take medication as prescribed. They may also need to attend additional appointments with their healthcare team to monitor their progress and manage any ongoing issues. With proper care and management, most patients are able to recover and return to normal activities after a Whipple surgery.
Choosing your surgeon: Why Dr. Babak Eghbalieh for your Whipple procedure?
Finding the best surgeon for a Whipple procedure can be a complex process. It is important to look for a surgeon who has experience and expertise in performing this type of surgery, as it is a highly specialized procedure.
Some factors to consider when selecting a surgeon for a Whipple procedure include:
- Experience: Look for a surgeon who has performed many Whipple procedures and has a high success rate.
- Credentials: The surgeon should be board-certified in general surgery and have additional training and experience in pancreatic surgery.
- Hospital affiliation: The surgeon should be affiliated with a hospital that has a dedicated pancreas center and a multidisciplinary team of healthcare professionals.
- Referrals: Ask for referrals and testimonials from other healthcare professionals or patients who have had a Whipple procedure.
- Communication: Look for a surgeon who communicates effectively and takes the time to answer all of your questions and concerns.
Dr. Babak ‘Bobby’ Eghbalieh stands as a distinguished figure in the surgical treatment of pancreatic cancer, bringing an unparalleled depth of expertise and dedication to each Whipple procedure he performs. With his advanced training in hepatobiliary pancreatic surgery and pioneering role in robotic surgery, Dr. Eghbalieh embodies the pinnacle of surgical precision and innovation. His leadership as Director of Robotic Surgery at PHCMC and extensive experience with over 15,000 operations, including more than 2,000 robotic surgeries, mark him as a leading authority in the field. His commitment to providing personalized, state-of-the-art care is evidenced by his pivotal role in establishing the first Pancreatic Cancer Center of Excellence in Los Angeles. Patients under Dr. Eghbalieh’s care benefit from his vast surgical prowess, compassionate bedside manner, and the multi-disciplinary approach he champions—ensuring that each patient receives the most comprehensive and effective treatment available.
Contact SCMSC
Take the vital step towards your healing journey with a trusted expert in Whipple surgery. Contact Southern California Multi-Specialty Center today to schedule a consultation, and experience the compassionate, cutting-edge care that sets our practice apart.
Our Expert General & Robotic Surgery Team
SCMSC’s board-certified surgeons bring advanced training and focused experience across a wide range of general surgical procedures. We believe informed patients make stronger decisions, and we welcome second opinions when facing important surgical choices. Every recommendation is made with clarity, precision, and your long-term health in mind.
Babak (Bobby) Eghbalieh, M.D., FACS
David Wang, MD

Seong (Sam) Gon Bae, M.D., FACS