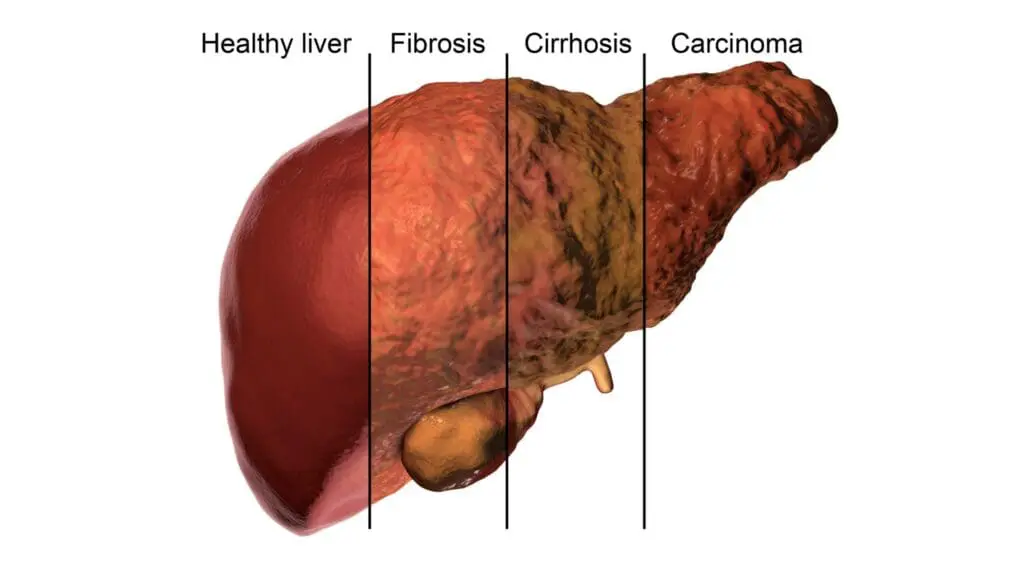
SCMSC’s Fatty Liver Surveillance Program
If you, or a loved one, has been diagnosed with Non-Alcoholic Fatty Liver Disease, you understandably want to monitor the condition closely.
After all, about 10% to 30% of people with this disease have an early stage of Hepatocellular Carcinoma (HCC) which is the third leading cause of cancer death in the United States, and growing yearly.
Southern California Multi-Specialty Center has a comprehensive surveillance program for non-alcoholic fatty liver disease to identify and intervene if the disease progresses to hepatocellular cancer.
This program was developed by one of the leading surgeons in the state of California. To find out if you or a loved one qualifies for this program call 818.900.6480 now.
If you want to understand the disease and the surveillance program in greater detail, keep reading. In this article we will discuss the risk factors, progression to cirrhosis, the role of alcohol and genetics, and provide details about the non-alcoholic fatty liver surveillance program.
Clinical Update
In 2023, global health organizations officially renamed Non-Alcoholic Fatty Liver Disease (NAFLD) to Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD) to more accurately reflect how metabolic health, like diabetes and heart health, impacts the liver. At SCMSC, we use this framework to provide more targeted, life-saving care.
Do you have fatty liver disease and don’t know it?
Fatty liver disease is silent by design. The liver has no pain receptors, which means significant damage can accumulate for years before any symptom appears. By the time most patients are diagnosed, the disease has already been progressing quietly in the background.
The question isn’t whether you feel sick. The question is whether your liver has already started down a path you haven’t been told about yet.
Could this be you? A simple risk check
- Have you been told you have a “fatty liver” on an ultrasound, CT scan, or MRI — even in passing?
- Do you have Type 2 diabetes or pre-diabetes?
- Is your BMI over 27, or have you struggled with weight around your midsection?
- Do you have high cholesterol, high triglycerides, or high blood pressure?
- Have you been diagnosed with metabolic syndrome?
- Are you of Hispanic or Asian descent? (Both carry elevated genetic risk)
- Are you over 45 years old with any of the above?
- Do you have a family history of liver disease or liver cancer?
Already scheduled for gallbladder surgery?
This one surprises most patients: if you’re already scheduled for gallbladder removal (cholecystectomy), you may be sitting on a major diagnostic opportunity.
Gallstone disease and fatty liver disease share nearly identical risk factors — obesity, diabetes, metabolic syndrome — which means a large percentage of patients coming in for gallbladder surgery also have undiagnosed liver disease. Because the surgeon already has direct visualization of your liver during the procedure, a small needle biopsy can be performed at the same time, at minimal additional risk, to definitively stage your liver health.
This single step — an opportunistic liver biopsy during a procedure you’re already having — can provide more accurate information about your liver than any blood test or imaging study alone. It tells us your exact fibrosis stage, whether NASH is present, and how urgently surveillance or intervention is needed.
If you have an upcoming abdominal surgery and any of the metabolic risk factors above, ask us about adding a liver assessment to your surgical plan. It could be the most important thing that happens in that operating room.
Why act now, before you have symptoms?
Liver cancer caught early — before symptoms appear, while it’s still a single small lesion — carries a 5-year survival rate above 70%. Liver cancer caught late, when it has grown or spread, carries a 5-year survival rate below 15%.
The cancer hasn’t changed. The outcome has — entirely because of when it was found.
There is no pain that tells you when fatty liver becomes NASH. No alarm that sounds when NASH becomes fibrosis. No symptom that announces the transition to cirrhosis. The only way to know where you are on that spectrum is to look — proactively, systematically, before anything goes wrong.
That is exactly what this program is designed to do.
The best time to evaluate your liver was years ago. The second best time is now.
Think you might be at risk?
You don’t need a diagnosis or a referral to reach out. Call us at (818) 900-6480 or request an appointment online. A single evaluation can tell you exactly where your liver health stands — and give you a clear plan for what comes next.
The Prevalence of HCC in NAFLD
Non-Alcoholic Fatty Liver Disease (NAFLD) impacts more than 25% of the US and global population. About 25% of those individuals progress to nonalcoholic steatohepatitis (NASH). NASH can result in progressive hepatic fibrosis, cirrhosis, and hepatocellular carcinoma (HCC).
About 90% of patients diagnosed with NAFLD have steatosis that is relatively benign but has an overall low mortality rate of 6–8%. However, about 10-30% of those affected have an early stage form of NAFLD non-sympathetic autoimmune disease.
What This Means for You: In simpler terms, while a large portion of the population has “fatty liver,” the condition is a sliding scale. Most cases stay quiet and manageable (benign), but for about 1 in 4 people, the liver begins to transition from simple fat buildup to active inflammation (NASH). Left unmanaged, this inflammation can create internal scarring (fibrosis) that eventually leads to more serious risks like cirrhosis or liver cancer (HCC).
Our program is designed to identify exactly where you are on this timeline. By catching the “silent” transition from simple fat to active inflammation early, we can often halt or even reverse the damage before it reaches a critical stage.
Beyond the diagnosis: understanding MASLD and Hepatocellular Health
In the past, these conditions were often grouped under the broad umbrella of “Fatty Liver.” Today, by using the more precise framework of Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD), our specialists can look closer at the WHY behind the condition. Whether you are concerned about persistent inflammation or have been told you are at risk for hepatocellular complications, the shift to MASLD means we are looking at your liver health in the context of your whole body… your metabolism, your heart, and your lifestyle.
At SCMSC, we don’t just treat a diagnosis; we treat a person. If you’ve been searching for answers about liver scarring or disease progression, know that MASLD is a condition where early, expert intervention can make a profound difference. We are here to help you navigate from uncertainty to a clear, actionable plan for protection and recovery.
Risk of non-alcoholic fatty liver disease increases with obesity, type 2 diabetes, high blood pressure, high cholesterol, metabolic syndrome, sleep apnea and a sedentary lifestyle.
What is this surveillance program?
As with other chronic noncirrhotic liver diseases, follow-up of NAFLD (Non-Alcoholic Fatty Liver Disease) patients should consist of monitoring biochemical, metabolic and body weight parameters every 6 months and performing abdominal ultrasound every 6 months.
At SCMSC enrollment in the inclusive surveillance program consists of the following:
- Ultrasound every 6 months for 2 years and then yearly after that
- Fasting bloodwork every 6 months for 2 years and then yearly after that
- Custom nutrition plan based on your specific dietary needs from our in-house specialty dietician
- Lifestyle modification plan
- Proprietary supplementation plan customized for each patient to promote liver regeneration and reversal of disease
The surveillance window: why 6 months matters
Research has shown that fibrosis — the internal scarring that drives this disease toward cirrhosis and cancer — can advance by a full stage in as little as two years. In some patients, the progression from early NASH to cirrhosis has been documented in under 24 months.
HCC has an estimated tumor doubling time of approximately 117 days, meaning a tumor can double in size roughly every 4 months. A 6-month surveillance interval is therefore the clinically validated sweet spot: short enough to catch tumors while they remain within curative size thresholds (under 2 cm), long enough to be practically sustainable for patients and health systems.
A once-yearly ultrasound doesn’t just create a gap in your monitoring. In a disease that moves this fast, it creates a blind spot wide enough for the trajectory of your liver health to change completely between visits — without anyone knowing.
This is precisely why the American Association for the Study of Liver Diseases (AASLD), the European Association for the Study of the Liver (EASL), and the Asian Pacific Association for the Study of the Liver (APASL) — three of the most respected liver disease organizations in the world — have independently arrived at the same conclusion: high-risk patients need liver surveillance every six months, not every twelve.
That consensus isn’t coincidence. It reflects decades of research showing that liver cancer in the setting of fatty liver disease grows quickly enough that a 12-month window is simply too long. Tumors that are detectable and curable at 6 months can be inoperable by 12. The difference between those two outcomes isn’t the cancer — it’s the calendar.
Our biannual ultrasound protocol exists for one reason: to make sure that when something changes in your liver, we find it while we can still do something about it.
Twice a year is not excessive. In this disease, it is the minimum responsible standard of care.
Geoffrey Samson, MS, RD
Director of Clinical Nutrition, Regenerative Medicine Program
Why Nutrition Matters as Part of Treatment
Food patterns can reduce liver fat
Mediterranean and plant-forward eating patterns—rich in fiber, polyphenols, and healthy fats—are associated with reduced liver fat and improved liver enzymes, even with modest weight loss.
A more complete approach to care
When nutrition or lifestyle factors can strengthen the body’s response to treatment, they’re thoughtfully considered as part of the care plan. This broader perspective helps our patients feel supported, informed, and set up for healthier progress at every stage of treatment.
Learn how nutrition is considered in your care →
REFERENCES
- Meir AY, et al. Green-Mediterranean diet and intrahepatic fat (DIRECT-PLUS). Gut. 2021;70:2085–2095.
- EASL-EASD-EASO Clinical Practice Guidelines on MASLD. Journal of Hepatology. 2024.
A precision, risk-stratified approach to fatty liver disease (MASLD)
At SCMSC, we do not treat fatty liver disease as a binary diagnosis.
We use a precision, risk-stratified model to determine which patients have simple steatosis and which may have metabolically active steatohepatitis (MASH/NASH) or early fibrosis — the stage of disease that carries long-term risk.
While many patients can be monitored safely using advanced blood-based markers and imaging tools, select individuals benefit from definitive histologic staging to guide long-term surveillance and prevention strategies.
Non-Alcoholic Fatty Liver Disease Q&A
Symptoms of NAFLD may include abdominal swelling (ascites), enlarged blood vessels just beneath the skin’s surface, enlarged spleen, red palms and yellowing of the skin and eyes (jaundice).
What are the risk factors for NAFLD?
- Obesity: Overweight or obese patients have the most significant risk factor for NAFLD. The excess body fat can lead to the accumulation of fat in the liver.
- Type 2 diabetes: People with type 2 diabetes are at higher risk of developing NAFLD because of insulin resistance.
- High blood pressure: High blood pressure can damage the liver and increase the risk of NAFLD.
- High cholesterol and triglycerides: Elevated levels of cholesterol and triglycerides in the blood can lead to the development of NAFLD.
- Metabolic syndrome: This is a cluster of conditions that include obesity, high blood pressure, high blood sugar, and high cholesterol levels. People with metabolic risk factors are at higher risk of developing NAFLD.
- Sleep apnea: People with sleep apnea, a condition where breathing repeatedly stops and starts during sleep, are at higher risk of developing NAFLD.
- Sedentary lifestyle: Lack of physical activity can increase the risk of NAFLD.
- Age: NAFLD is more common in people over 50 years old.
- Genetics: Certain genetic mutations can increase the risk of NAFLD.
It is important to note that not everyone with these risk factors will develop NAFLD, and some people without any risk factors may still develop the condition.
What are the risk factors for Cirrhosis?
there are several risk factors that have been identified:
- Alcohol abuse: Heavy and prolonged alcohol consumption is the most common cause of cirrhosis.
- Chronic viral hepatitis: Chronic hepatitis B or C can cause inflammation and damage to the liver, which can lead to cirrhosis.
- Non-alcoholic fatty liver disease: Accumulation of fat in the liver, known as non-alcoholic fatty liver disease (NAFLD), can progress to cirrhosis in some cases.
- Autoimmune hepatitis: An autoimmune disorder where the immune system attacks liver cells, leading to inflammation and damage, can cause cirrhosis.
- Primary biliary cholangitis: A disease that causes inflammation and damage to the small bile ducts in the liver, leading to cirrhosis.
- Primary sclerosing cholangitis: A disease that causes inflammation and scarring of the bile ducts in the liver, leading to cirrhosis.
- Hemochromatosis: A genetic disorder where the body accumulates too much iron, which can damage the liver and lead to cirrhosis.
- Wilson’s disease: A rare genetic disorder where the body accumulates too much copper, which can damage the liver and lead to cirrhosis.
- Nonalcoholic steatohepatitis (NASH): A severe form of non-alcoholic fatty liver disease that involves inflammation and damage to liver cells, leading to cirrhosis.
- Chronic exposure to toxins: Exposure to certain chemicals, such as those found in pesticides, can lead to cirrhosis.
It is important to note that not everyone with these risk factors will develop cirrhosis, and some people without any risk factors may still develop the condition. Early diagnosis and management of these risk factors can help prevent or delay the development of cirrhosis.
What Is the definition of alcohol abuse?
According to the Centers for Disease Control and Prevention (CDC), heavy alcohol consumption is defined as consuming more than 14 drinks per week for men and more than 7 drinks per week for women. Prolonged alcohol consumption refers to drinking at this level for an extended period of time, typically for years.
It is important to note that heavy and prolonged alcohol consumption can vary based on factors such as body mass index, age, and health status. Additionally, even lower levels of alcohol consumption can contribute to the development of liver diseases and other health problems over time, especially in people who are susceptible to the effects of alcohol.
Timing: NAFLD to Cirrhosis
An old school of thought was that progression from the early stage of patients with NAFLD to cirrhosis took decades, but recent studies have shown that some people this chronic liver disease progresses rapidly within 2 years. However, research has also shown that there is reversibility, which is why Dr. Bobby Eghbalieh created this fatty liver disease surveillance program.
Make an Appointment
You are not alone in this health journey. The SCMSC team in LA is always here, blending professional expertise with a touch of human understanding.
To schedule an evaluation with Dr. Eghbalieh at Southern California Multi-Specialty Center, call 818-900-6480.
Our Expert General & Robotic Surgery Team
SCMSC’s board-certified surgeons bring advanced training and focused experience across a wide range of general surgical procedures. We believe informed patients make stronger decisions, and we welcome second opinions when facing important surgical choices. Every recommendation is made with clarity, precision, and your long-term health in mind.
Babak (Bobby) Eghbalieh, M.D., FACS
David Wang, MD

Seong (Sam) Gon Bae, M.D., FACS