The SCMSC Pancreatic Cyst Surveillance Program
At SCMSC, pancreatic cyst surveillance is not a one-size-fits-all protocol. It is a structured, individualized program built around your specific cyst characteristics, your risk profile, and your overall health — with the surgical expertise to act decisively if and when action is ever needed.
How the Program Works

Step 1: Comprehensive Initial Evaluation
Your first visit begins with a thorough review of any existing imaging, your medical history, and the specific features of your cyst. Not all pancreatic cysts carry the same risk, and the first goal is to accurately characterize what you have. Size, location, cyst type, ductal involvement, the presence of any solid components — all of these factors determine how urgently your cyst needs to be monitored and what modality gives us the clearest picture.
Step 2: Individualized Imaging — The Right Tool for Your Cyst
Depending on your cyst’s characteristics, we use one or more of the following imaging modalities:
MRI with MRCP (Magnetic Resonance Cholangiopancreatography) is our primary surveillance tool for most pancreatic cysts. It provides exceptional soft tissue detail, clearly visualizes the pancreatic duct, and — critically — involves no radiation, making it safe for the repeated imaging that long-term surveillance requires.
CT scan is used when rapid, detailed anatomic assessment is needed, particularly when a cyst has changed or when surgical planning is under consideration.
Endoscopic Ultrasound (EUS) gives us the highest resolution view of a cyst’s internal architecture — wall thickness, septations, mural nodules — and when a cyst has features that warrant it, EUS allows us to perform Fine Needle Aspiration (FNA) to sample the cyst fluid directly. Fluid analysis can identify whether a cyst is mucinous, assess for malignant cells, and measure CEA levels within the cyst — information no external imaging can provide.
Step 3: Surveillance Intervals Matched to Your Risk
Pancreatic cyst surveillance is not a fixed schedule — it is a living protocol that evolves as your cyst does.
In the early phase of monitoring, we typically image every 3 to 6 months. This closer interval is intentional. The first one to two years of surveillance are the most important period for establishing your cyst’s behavior — whether it is stable, slowly changing, or showing features that demand a faster response. We want to know how your cyst acts before we make any long-term assumptions about it.
For patients whose cysts demonstrate consistent stability over time — no growth, no new solid components, no ductal changes, no worrisome features on serial imaging — we transition to annual surveillance. This reflects both the current evidence and a straightforward clinical reality: a cyst that has proven itself stable over multiple surveillance cycles carries a meaningfully different risk profile than one we are seeing for the first time. Extending the interval for stable, low-risk cysts is not a relaxation of care. It is the appropriate, evidence-based response to reassuring data.
That said, no cyst is permanently low-risk by assumption. If anything changes — growth in size, new internal features, a shift in your tumor markers, or new symptoms — the interval tightens immediately and we reassess the full picture. Stability is earned through surveillance, and it can be reconsidered at any point if the cyst gives us reason to look more closely.
An Added Layer: The Galleri® Multi-Cancer Early Detection Test
For patients who want the most comprehensive picture of their cancer risk available today, SCMSC offers access to the Galleri® test by GRAIL as an optional addition to our pancreatic cyst surveillance program.
The Galleri test is a simple blood draw that analyzes cell-free DNA circulating in the bloodstream to detect cancer signals across more than 50 cancer types — including pancreatic cancer — often before any symptoms are present. What makes it particularly relevant for our pancreatic cyst patients is this: pancreatic cancer is one of the deadliest cancers precisely because it is almost never caught early through conventional means. The Galleri test is specifically designed to find signals from cancers like pancreatic, liver, and ovarian cancer — the ones that typically go undetected until it is too late.
For a patient already under pancreatic cyst surveillance, adding Galleri creates a second, entirely independent layer of detection. Imaging tells us what your cyst looks like. The Galleri test tells us what your blood is signaling — a complementary source of information that no scan alone can provide.
A few important things to know about the Galleri test:
- It is available by prescription only and offered as an optional add-on to your surveillance program
- It has demonstrated an overall sensitivity of 83.7% for pancreatic cancer across all stages in clinical studies, with a very low false positive rate of 0.4%
- It is not a replacement for imaging surveillance — it works alongside it
- It is currently available as a laboratory-developed test through GRAIL’s CLIA-certified laboratory; a full FDA premarket approval application was submitted in January 2026 and is currently under review
- It is recommended for adults 50 years and older, or those with elevated cancer risk
This is not a test we offer to everyone. We offer it to patients for whom we believe the additional clinical information is genuinely meaningful — and we interpret the results in the context of everything else we know about your cyst, your markers, and your overall health picture.
This risk-stratified, adaptive approach is grounded in the current guidelines of the American Gastroenterological Association (AGA), the International Association of Pancreatology (IAP), and the American College of Gastroenterology — all of whom recognize that surveillance frequency must reflect what the cyst is actually doing, not simply how long the patient has been in the program.
Step 4: Bloodwork and Tumor Markers
Regular laboratory evaluation is integrated into every surveillance visit. This includes CA 19-9 — a tumor marker that, when elevated, can signal malignant transformation — as well as CEA and a broader metabolic panel. While no single blood test can diagnose pancreatic cancer, trends in these markers over time provide important clinical signals that imaging alone may not capture. We track these values longitudinally, looking for patterns rather than isolated readings.

Step 5: Nutrition and Lifestyle Optimization
Emerging research suggests that metabolic health — specifically obesity, insulin resistance, and chronic inflammation — plays a meaningful role in the behavior of pancreatic cysts and pancreatic cancer risk more broadly. Our program includes access to SCMSC’s in-house registered dietitian, who works with patients on dietary patterns shown to reduce systemic inflammation and support overall pancreatic health. This is not a generic handout. It is a personalized nutritional plan built around your specific health profile.

Step 6: Surgical Evaluation When It Matters
The majority of pancreatic cysts will never require surgery. But for those that do — cysts that grow beyond 3 cm, develop high-risk features, or show cytological evidence of dysplasia or malignancy — having a surgeon leading your surveillance program rather than a generalist is a decisive advantage.
Dr. Eghbalieh is not only monitoring your cyst. He is evaluating it with a surgeon’s eye at every visit — assessing resectability, planning operative approach, and ensuring that if the moment for intervention arrives, you are already in the hands of someone who can act. There is no referral delay. No handoff to an unfamiliar team. No time lost.
Who should be in this program
You may be a candidate for the SCMSC Pancreatic Cyst Surveillance Program if:
- A cyst was found incidentally on a CT, MRI, or ultrasound performed for another reason
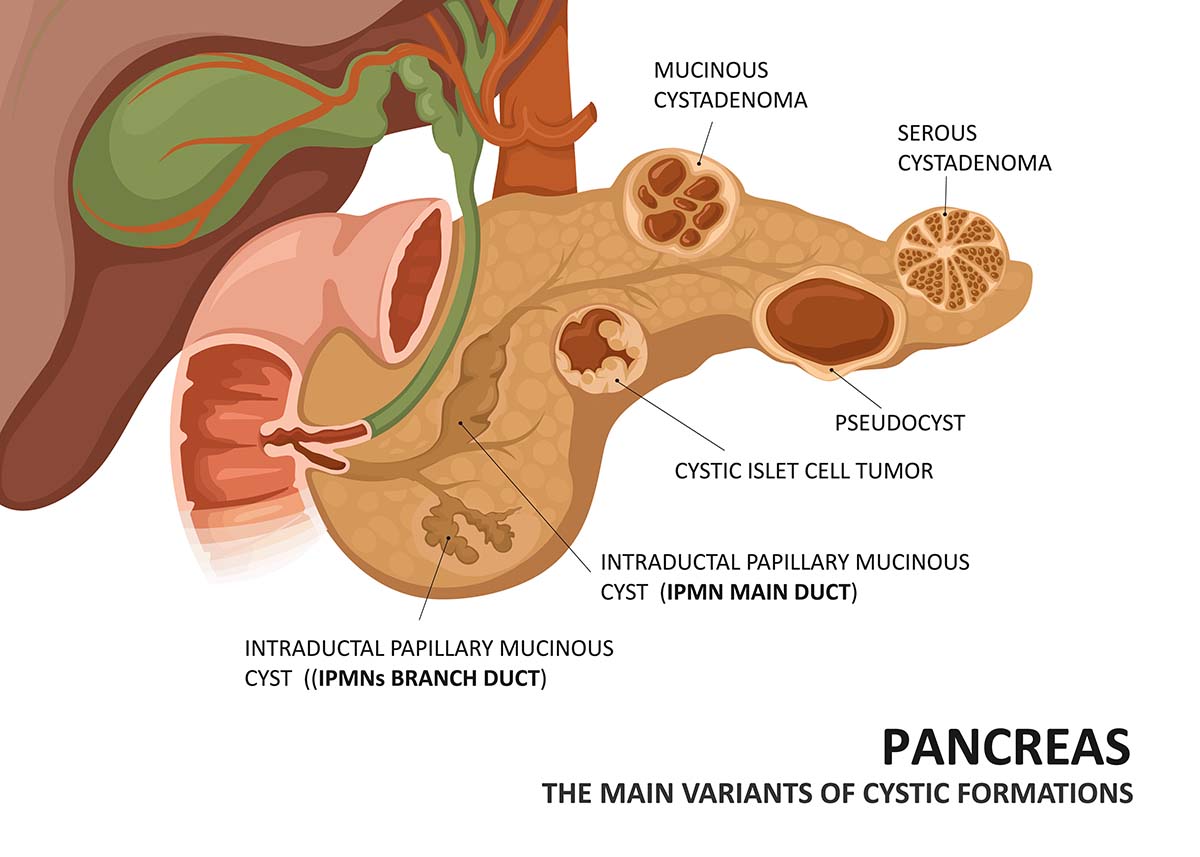
- You have been diagnosed with an IPMN (intraductal papillary mucinous neoplasm), MCN (mucinous cystic neoplasm), or other pancreatic cystic lesion
- You have a family history of pancreatic cancer
- You have a known genetic syndrome associated with pancreatic cancer risk (BRCA1/2, Lynch syndrome, Peutz-Jeghers, familial atypical mole melanoma)
- You were previously told your cyst was “benign” or “nothing to worry about” but have never had structured follow-up
- You are seeking a second opinion on a cyst that has been identified elsewhere
You do not need a referral to be seen. If you have imaging showing a pancreatic cyst and you want expert surgical eyes on it, call us directly.
Why Surgical Expertise Changes Everything
Most pancreatic cyst surveillance programs are run by gastroenterologists — physicians who are expert at imaging interpretation and endoscopy, but who do not perform the surgery if a cyst becomes cancerous. At SCMSC, your surveillance is led by a fellowship-trained surgical oncologist who operates on the pancreas.
That distinction matters. When your surgeon is also your surveillance physician, every imaging finding is interpreted not just diagnostically, but operatively. The question being asked at every visit is not only “has this changed?” but “if this has changed, what do we do next — and are we ready to do it?”
That is the difference between a monitoring program and a program that is genuinely built to save your life.
Schedule an Evaluation
The SCMSC team in LA is always here, blending professional expertise with a touch of human understanding. To schedule your initial evaluation, call Southern California Multi-Specialty Center at 818-900-6480 or request an appointment online. No referral required..
Frequently Asked Questions
Do all pancreatic cysts need to be monitored?
When do you stop surveillance pancreatic cysts?
How are pancreatic cysts monitored?
Followed by MRI testing every one or two years.
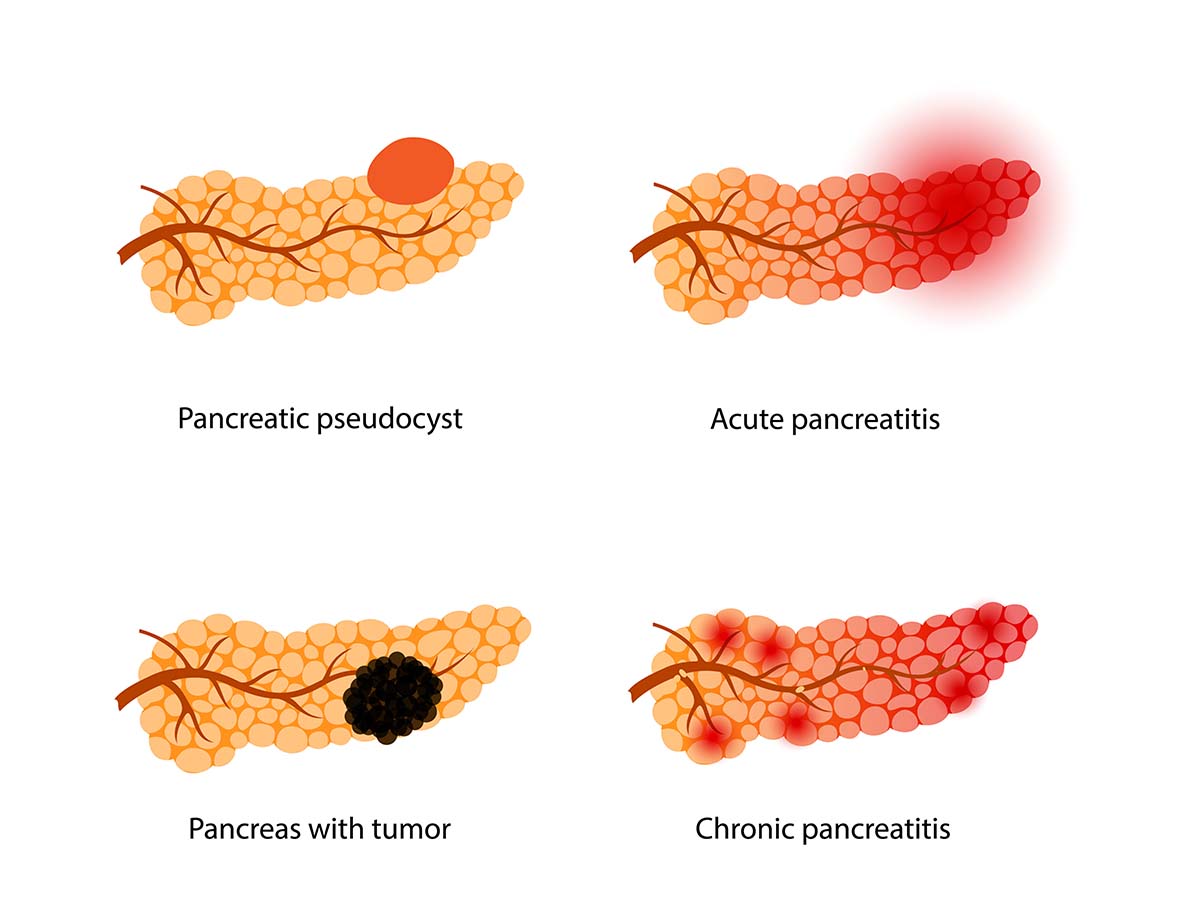
What are the different types of pancreatic cysts?
What are the high-risk features of pancreatic cysts?
Our Expert General & Robotic Surgery Team
SCMSC’s board-certified surgeons bring advanced training and focused experience across a wide range of general surgical procedures. We believe informed patients make stronger decisions, and we welcome second opinions when facing important surgical choices. Every recommendation is made with clarity, precision, and your long-term health in mind.
Babak (Bobby) Eghbalieh, M.D., FACS
David Wang, MD

Seong (Sam) Gon Bae, M.D., FACS