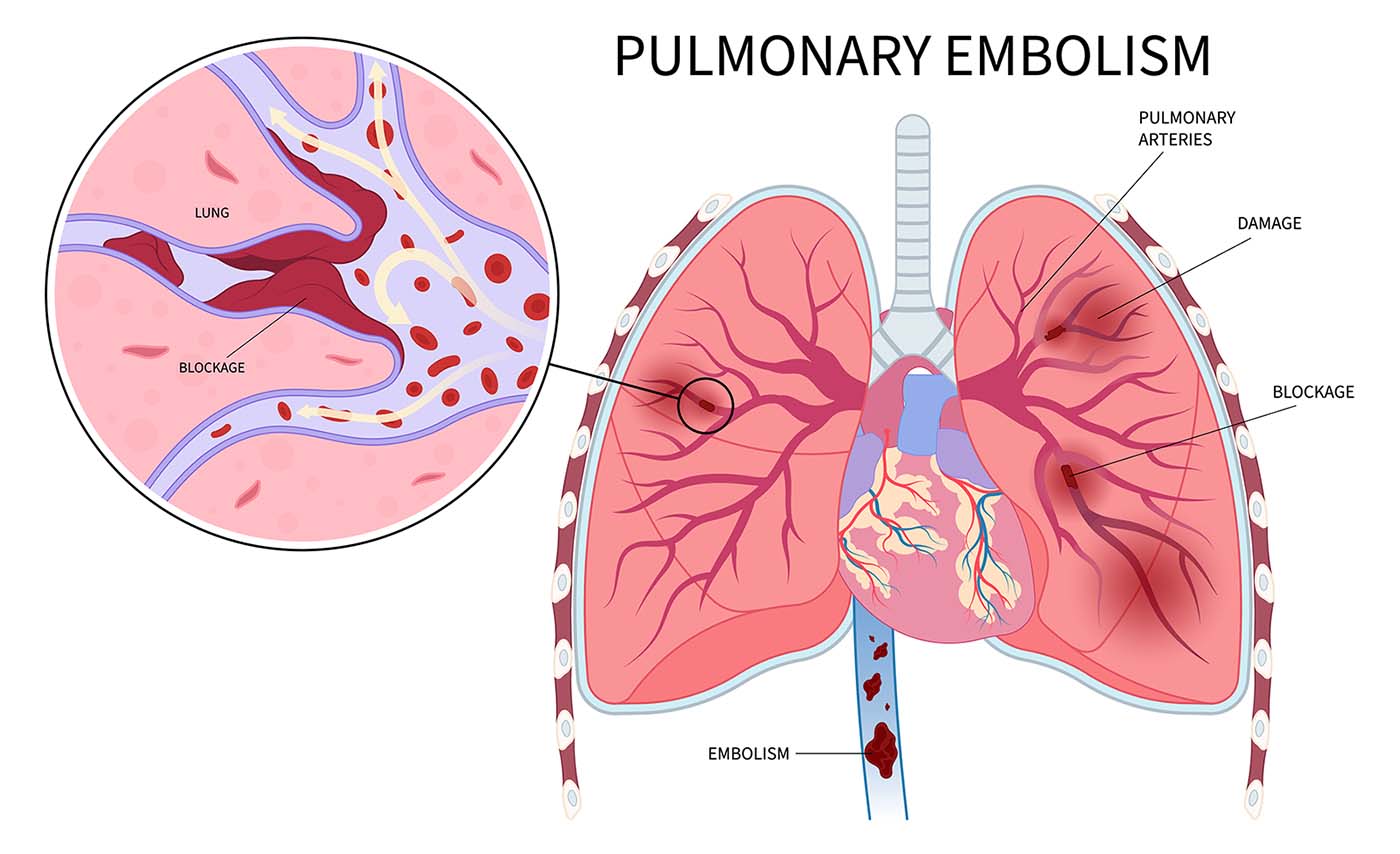
What is a Pulmonary Embolism?
An embolus is a blood clot that breaks off and moves to another part of the body. If that clot or embolus ends up traveling to the lungs, it is called a pulmonary embolism (PE). The clot can restrict blood flow to the lungs. This event can be life threatening if not treated immediately. Since PE is generally linked to deep vein thrombosis (DVT) the combined condition is called venous thromboembolism (VTE).
Risk factors for Pulmonary Embolism
Some people are more likely to develop a blood clot that can travel to the lungs and cause a pulmonary embolism. If any of the risk factors below apply to you, talk with your doctor about your personal risk and what you can do to lower it.
- Smoker
- Pregnant or postpartum up to 6 weeks
- History of heart failure or stroke
- History of deep vein thrombosis
- Varicose veins
- Birth control or hormone therapy
- Obese
- Sitting or inactive for a long period of time
- History of clots
- Cancer or chemotherapy
How a Pulmonary Embolism develops
A pulmonary embolism almost always starts somewhere else in the body. In many cases, a blood clot forms in the deep veins of the legs or pelvis, a condition called deep vein thrombosis or deep vein thrombosis (DVT). These deep veins carry blood back toward the heart. When a piece of that clot breaks off, it can travel through the inferior vena cava into the heart and then into the pulmonary arteries in the lungs. That moving clot is called a pulmonary embolus, and the event is known as pulmonary thromboembolism.
Together, deep vein thrombosis and pulmonary embolism are called venous thromboembolism. Certain medical conditions and lifestyle factors make it easier for clots to form, including long periods of bed rest, major surgery, cancer, hormone replacement therapy, birth control pills with estrogen, obesity, and inflammatory bowel disease. People with a family history of blood clots or inherited clotting problems also have an increased risk. When these risk factors are present, it’s easier for clot formation to occur and for a pulmonary embolism to start silently before symptoms appear.
How doctors diagnose a Pulmonary Embolism
When someone comes in with possible pulmonary embolism symptoms, doctors move quickly to decide how likely a PE is and which tests are needed. Diagnosis is built on three pieces: what you feel, what the exam shows, and what the tests reveal.
Symptoms of Pulmonary Embolism
A pulmonary embolism can look different from person to person, but common symptoms of a pulmonary event include:
- Sudden shortness of breath that gets worse with exertion
- Coughing up blood
- Fever
- Fainting
- Lightheaded / dizzy
- Chest pain that gets worse with coughing or deep breath
- Irregular or fast heartbeat
A Physical Exam
During the physical exam, your doctor checks your blood pressure, heart rate, and oxygen levels and looks for signs of deep vein thrombosis in the legs, such as swelling, warmth, or tenderness. These clinical symptoms and findings help determine your baseline PE diagnosis risk before ordering imaging tests or blood tests.
Imaging and Blood Tests
If a pulmonary embolism is suspected, your care team may use:
- Blood tests – A D-dimer test can help rule out PE in people with a low clinical probability. Other blood tests may look for markers of heart strain and overall clotting status.
- CT pulmonary angiography (CTPA) – This is the most common test used today. It uses contrast dye to create detailed pictures of the pulmonary arteries so doctors can see blood clots blocking blood flow.
- Ventilation–perfusion (V/Q) scan – Sometimes called a V Q scan, this compares air flow and blood flow in the lungs and can be useful when CT pulmonary angiography is not ideal.
- Ultrasound of the legs – Looks for clots in the deep veins; finding a clot supports the diagnosis when symptoms match pulmonary embolism.
- Pulmonary angiography – In select cases, a catheter-based pulmonary angiogram is used to precisely map clots in the main pulmonary artery and smaller pulmonary emboli and may guide advanced treatment.
These tests help your doctors see where blood flow is blocked, how much lung tissue is affected, and whether the heart is under strain so they can tailor the right pulmonary embolism treatment for you.
Treatment, recovery, and life after Pulmonary Embolism
The initial goal of treatment is to stabilize you, protect your heart and lungs, and stop the clot from getting larger. From there, the focus turns to recovery and long-term health.
Treatment Options for Pulmonary Embolism
Depending on the severity of your case, your physician may be able to treat your PE with blood thinners or IV clot-busting medications. However, in more severe cases, you may require surgical treatment.
The surgery options for a pulmonary embolism include:
- Pulmonary embolectomy
Surgical removal of the pulmonary embolisms. - Percutaneous thrombectomy (EKOS, Penumbra, Inari)
The use of a catheter to the site of the embolism by using X-ray guidance. The catheter is a long, thin, hollow tube.
What Recovery Can Look Like
Many people want to know if their lungs will heal after a pulmonary embolism and what their life expectancy will be. In most cases, lung tissue recovers as blood flow improves, and people return to normal or near-normal activities over weeks to months. Fatigue and shortness of breath can linger for a while but usually improve as the clot shrinks and the pulmonary circulation opens up again.
A small number of patients develop chronic thromboembolic pulmonary hypertension (CTEPH), where leftover clot and scar tissue cause ongoing high pressure in the pulmonary circulation and strain the heart. This complication is uncommon, but when it happens, it requires specialized care and sometimes advanced procedures to reopen the blocked blood vessels. Your SCMSC team watches closely for this and works with specialists if pulmonary hypertension becomes a concern.
Preventing future blood clots and Pulmonary Emboli
Once you’ve had a pulmonary embolism, preventing another one becomes a key part of your care plan. Prevention includes both lifestyle choices and medical interventions.
Everyday Steps to Improve Blood Flow
Simple, consistent habits can reduce your chance of developing blood clots:
- Move regularly throughout the day and avoid long stretches of sitting or bed rest when your doctor says it’s safe to be active.
- On long trips, stand up, walk, or flex your feet and ankles every hour or two.
- Drink enough fluids and avoid tight clothing that restricts blood flow in the legs.
- Work with your doctor to manage high blood pressure, heart failure, and other medical conditions that affect your blood vessels and heart.
- Talk with your provider about alternatives if you use birth control pills or hormone replacement therapy that may increase clot risk.
Medical Prevention Strategies
Your healthcare provider may recommend additional steps, especially if you have higher risk factors or medical conditions that make clots more likely:
- Blood thinners for a period of time after a pulmonary embolism or certain surgeries
- Compression stockings to support deep veins in the legs and reduce swelling
- A vena cava filter in rare cases when blood thinners cannot be used safely, to catch clots traveling toward the lungs
These strategies are tailored to your overall risk profile, including age, family history, prior venous thromboembolism, and other cardiovascular disease. The goal is to prevent future pulmonary emboli while keeping treatment as safe as possible for you.
Why Nutrition Matters as Part of Treatment
Plant-forward eating supports vascular health
Healthier, plant-forward dietary patterns and lower intake of ultra-processed foods are associated with a lower risk of venous thromboembolism and improved inflammatory balance.
A more complete approach to care
When nutrition or lifestyle factors can strengthen the body’s response to treatment, they’re thoughtfully considered as part of the care plan. This broader perspective helps our patients feel supported, informed, and set up for healthier progress at every stage of treatment.
Learn how nutrition is considered in your care →
REFERENCES
- Guo J, et al. Healthy plant-based diet and VTE risk. JACC: Advances. 2024;3:100643.
- Yuan S, et al. Ultra-processed food intake and incident VTE. Clinical Nutrition. 2023;42:1281–1289.
Pulmonary Embolism Q & A
What is a Pulmonary Embolism?
An embolus is a blood clot that breaks off and moves to another part of the body. If that clot or embolus ends up traveling to the lungs, it is called a pulmonary embolism (PE). The clot can restrict blood flow to the lungs. This event can be life threatening if not treated immediately. Since PE is generally linked to deep vein thrombosis (DVT) the combined condition is called venous thromboembolism (VTE).
Can you recover fully from blood clots in the lungs?
How serious are blood clots in the lungs?
Who is most at risk for pulmonary embolism?
You are at higher risk if you have a history of deep vein thrombosis, recent major surgery or trauma, cancer, long periods of immobility, or a strong family history of blood clots. Medical conditions such as heart failure, inflammatory bowel disease, and certain clotting disorders also raise risk. If you have several of these risk factors, your doctor may recommend preventive blood thinners or compression stockings in higher-risk situations like hospital stays or long travel.
How can I lower my risk if I’ve already had a PE?
Our Vascular & Endovascular Surgeons
It's important to remember not all physicians are trained in advanced vascular and endovascular surgery. It’s a good practice to get multiple opinions and do research on the surgery and the physician.