Once you leave the surgery center, most of the healing work happens at home. How you care for your surgical wound in those first days and weeks can make a significant difference in your healing time, comfort, and risk of infection.
At Southern California Multi-Specialty Center (SCMSC) in Los Angeles, your surgeon and healthcare provider team will send you home with specific wound care instructions. This at home surgical wound care guide is here to help you understand what those instructions mean, what’s normal, and when to call for help.
These guidelines do not replace your surgeon’s orders. If anything here conflicts with your written instructions, follow your healthcare provider’s plan and contact the office with questions.
Why Surgical Wound Care at Home Matters
A surgical incision is a controlled cut, but your body treats it like any other injury that needs protection and time. Good surgical wound care at home helps:
- prevent infection and other complications
- support a smoother healing process and faster healing
- reduce swelling and pain around the wound area
- lower the chance of slow healing or a scar that doesn’t settle well
Most wounds from surgery heal well with proper care. Patients with diabetes, poor blood flow, smoking history, or deep wound surgery may have a higher risk of infection or delay healing, so their at-home routine is especially important.
Think of wound care as caring for both the wound and your whole body. Clean skin, good blood flow, smart nutrition, and rest all work together to support wound healing.

Wounds From Traditional and Robotic Surgery
Patients at Southern California Multi-Specialty Center often notice that their surgical wounds don’t look like the “big scar” they expected. Traditional open surgery usually involves one larger surgical incision, while robotic and minimally invasive surgery is done through several smaller cuts, each just wide enough for a camera or instrument. The size and number of incisions may look different on the skin, but every incision is still a surgical wound that needs proper care.
With minimally invasive and robotic procedures, many patients experience less overall pain, smaller scars, and faster healing time. Even so, the healing process inside your body is similar. Each wound area has to seal, rebuild tissue, and stay free from infection. Thus, the basics of at home surgical wound care stay the same for both traditional and robotic surgery.
The 4 C’s of Wound Care
We use a simple version of the “4 C’s” so patients and families can remember what matters most.
Clean
Keep the wound clean with mild soap and water or mild soapy water when your surgeon says it’s safe to wash. The goal is to gently clean around the wound without scrubbing or irritating the skin.
Cover
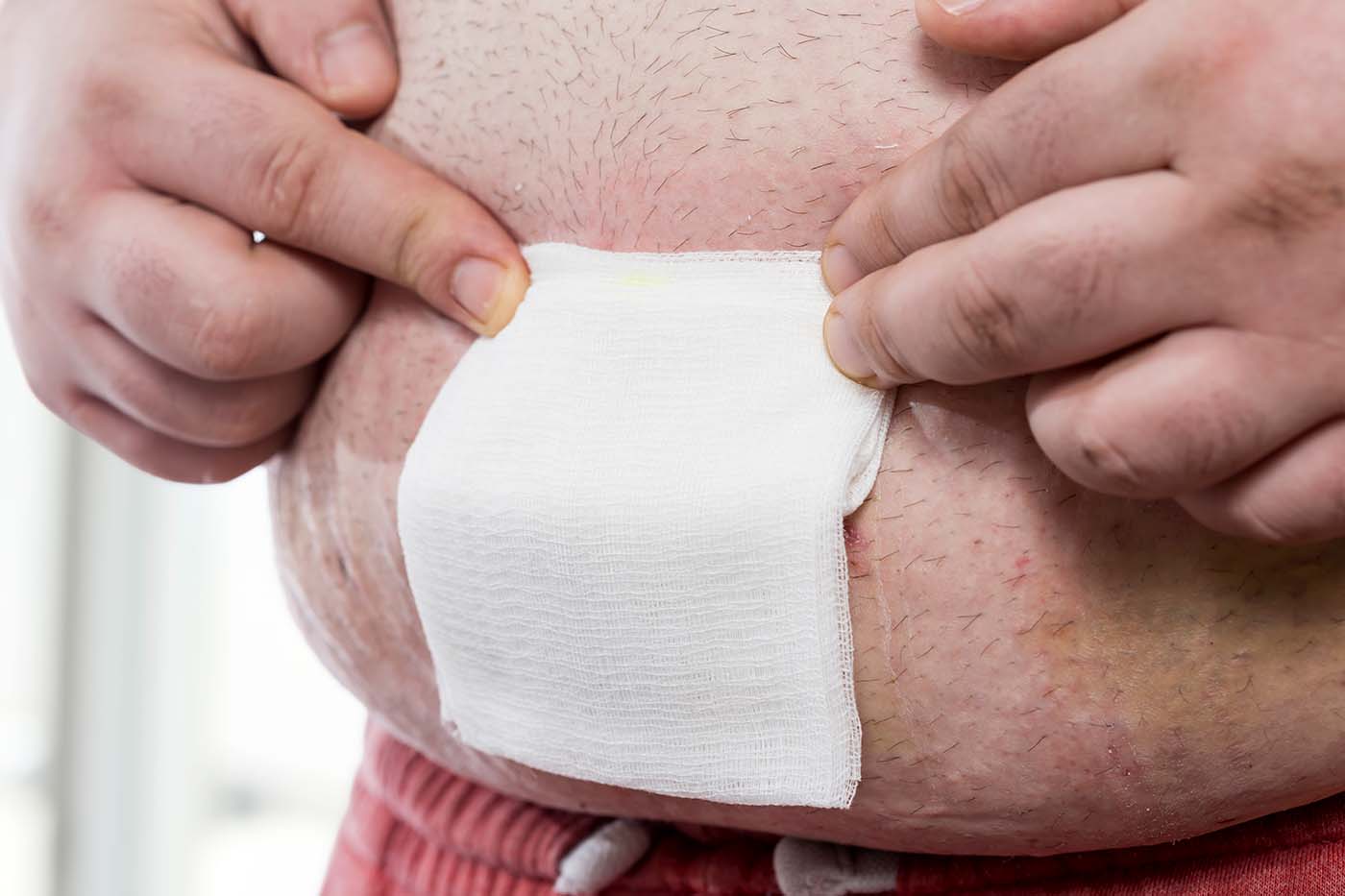
Use the bandage, gauze pad, adhesive bandage, or sterile dressing your team recommends. Covering a surgical wound helps keep the wound clean, prevents infection, and protects the skin from rubbing and friction.
Comfort
Watch for pain and swelling and follow your pain plan. Using ice packs as directed, elevating the area, and keeping the wound dry and protected can reduce swelling and help you move more comfortably.
Call
If something looks wrong or feels different such as more pain, increased redness, new bleeding, or any sign of infection, call your healthcare provider. Early medical attention can prevent small problems from becoming serious complications.
If you can remember Clean, Cover, Comfort, Call, you’ve got the core of proper at-home wound care.
Getting Ready at Home: Simple Wound Care Setup
Before surgery, or as soon as you get home, set up a small wound care station in an easy-to-reach spot. You don’t need a hospital supply closet, just a few key items:
You’ll typically want disposable medical gloves, a mild soap, a clean cloth or soft cloth, a clean towel, sterile dressing or gauze pads, medical tape or bandage materials, and any antibiotic ointment or other treatment your doctor prescribed to apply in a thin layer. Keeping these supplies together means you won’t be searching for a clean cloth or medical tape while you’re trying to change the dressing.
If you’re unsure which dressing or bandage to buy, ask your nurse before discharge or call the office for brand-agnostic guidance.

Step-by-Step: How to Gently Clean a Surgical Wound
Your surgeon will tell you when it’s safe to get the wound wet. Many patients can use soap and water or warm water on the surgical incision after the first 24–48 hours, but timing depends on your surgery.
A typical cleaning routine looks like this:
- Wash your hands with soap and warm water and dry them with a clean towel. If you’re using disposable medical gloves, put them on after you wash your hands with soap and water.
- Carefully remove the old dressing. Notice how much drainage is on the old dressing and what it looks like. A small amount of clear or slightly bloody fluid can be normal; pus or strong odor is not.
- Gently clean around the wound with mild soap and water, soapy water, or mild soapy water as directed. Use a soft cloth or clean cloth and gently wipe—don’t scrub. Avoid soaking the wound in a bath or hot tub unless your healthcare provider specifically instructs you to do so.
- Rinse with clean, warm water and pat the wound dry. Try to pat the wound dry instead of rubbing. The wound should be clean and the skin around the wound dry before you cover it.
- Check the wound area and the skin around the wound for increased redness, swelling, or new pain. If you see heavy bleeding, pus, or anything that looks very different from prior days, call your doctor.
Most wounds should not bleed heavily when you gently clean them. If you can’t stop bleeding with light pressure and a clean dressing, seek medical attention.
Covering the Wound: Do Surgical Wounds Heal Better Covered or Uncovered?
Many people wonder if it’s better to “let a wound breathe.” For a surgical wound, modern wound care usually favors staying covered:
A clean dressing or bandage protects the skin from bacteria, clothing, and everyday bumps. It helps keep the wound slightly moist, which can support new tissue and lead to faster healing. It also makes it easier to use ice packs or loose clothing without irritating the incision.
Your discharge instructions will outline how often to change the dressing and how long to keep your surgical incision covered. Some surgeries only need a light bandage for a few days, while others require dressing daily changes for one to two weeks.
Old dressing should always be thrown away in the trash, and you should wash your hands after handling it. If your bandage keeps getting wet, sliding off, or soaking through, reach out to your healthcare provider. Persistent wet dressings can delay healing and increase infection risk.
What Can I Put on a Surgical Wound to Help It Heal?
It’s tempting to use home remedies, oils, or store-bought skin cleansers on a surgical wound, but that can do more harm than good. In many cases, proper care means less is more.
Your doctor may recommend:
- plain soap and water for cleaning
- a thin layer of antibiotic ointment in certain high-risk areas
- manuka honey due to its potent antibacterial, anti-inflammatory, and tissue-regenerating properties
Strong products like full-strength hydrogen peroxide, harsh skin cleansers, or salt water rinses on fresh surgical wounds can damage new tissue and slow healing. Unless your instructions specifically mention a treatment, stick to mild soap, clean water, and whatever your surgeon prescribed.
If you’re thinking about using anything new such as a cream, spray, ointment, or essential oil, ask first. A quick phone call can prevent irritation, infection, or slow healing.
How Long Should I Keep My Surgical Incision Covered?
There isn’t a single rule for every surgery. The right healing time depends on the type of surgery, the location of the wound, and your personal risk factors.
Most wounds from routine surgery are kept covered for the first couple of days and then checked by your healthcare provider or at your follow-up visit. Some patients with deep wound repairs, higher infection risk, or incisions in high-friction areas (like under the breast or in body folds) may need dressing protection longer.
If your incision looks dry on the surface, that doesn’t always mean it’s ready to be uncovered. Stopping dressings too soon can increase risk of infection and complications, especially if clothing rubs the area or it stays wet with sweat. When you’re in doubt, ask before you change the plan.
When to Call About Your Surgical Wound
Healing should trend in one direction: better. A little soreness, mild swelling, and slight redness can be normal early on, but they should slowly improve.
Pay attention to patterns:
Pain and Redness
If you notice increased pain after several days of improvement or increased redness spreading away from the incision, that can be a sign of infection. Pain that suddenly spikes or burning pain around the wound deserves a call to your doctor.
Drainage and Bleeding
Thin, clear or slightly pink drainage on the dressing can be normal. Pus, thick yellow or green fluid, or bleeding that doesn’t stop when you cover the area with a clean dressing and light pressure needs medical attention.
Swelling, Heat, and Fever
Swelling close to the incision is common, but swelling that grows, feels hot, or comes with fever or chills is not. That’s especially important if you’ve had surgery on the leg or breast, where infection and fluid collections can be more serious.
If at any point you feel very sick, dizzy, or short of breath, don’t wait to see what happens. Go to the closest emergency room or call 911.
Special Situations and Higher-Risk Wounds
Some wounds need more careful follow-up. Open wounds in delicate areas, such as an open wound on the breast after surgery, should always be monitored closely by your surgeon. These areas can be harder to keep dry, are more prone to friction, and may have higher risk for slow healing.
Patients with diabetes, circulation problems, a history of poor wound healing, or those on medicines that affect the immune system need to be extra alert. If you fall into any of these groups, you’ll likely see your healthcare provider more often while the wound heals. Keep every appointment and speak up if anything feels off.
How SCMSC Supports Your At-Home Surgical Wound Care
You are not expected to manage surgical wound care alone. At Southern California Multi-Specialty Center, your surgeon, nurses, and support staff work together to:
- explain your wound care plan before you leave the surgery center
- show you and your caregiver how to gently clean and cover the wound
- clarify how often to change the dressing and what normal healing looks like
- help you know when slight wetness, bruising, or pain is okay and when it’s not
Because your whole body affects how your surgical wound heals, SCMSC also offers a dedicated Nutrition & Diet department. The team can help you choose foods and supplements that support blood flow, skin repair, and the healing process from before surgery through recovery, so your wound care routine works with your body, not against it.






